Many people who are elderly or who have disabilities, and still live at home, rely on home health workers. The workforce is composed of tens of thousands of Virginians, the vast majority of whom are women.
Nationwide the median income for home health workers is less than $25,000. Now these low wage workers are on the frontlines of a pandemic, and advocates worry they’re being overlooked.
Karen Acree is 61 and lives in South Boston, a small town near the North Carolina line. She’s a certified nurse assistant, and has three patients she regularly visits at home. That routine hasn’t stopped as COVID-19 has spread.
She describes one patient who she’s still visiting.
“He lives by himself, he goes on dialysis, he has one leg, you see?” she explained during a recent phone interview. “I have to go in there to check on him.”
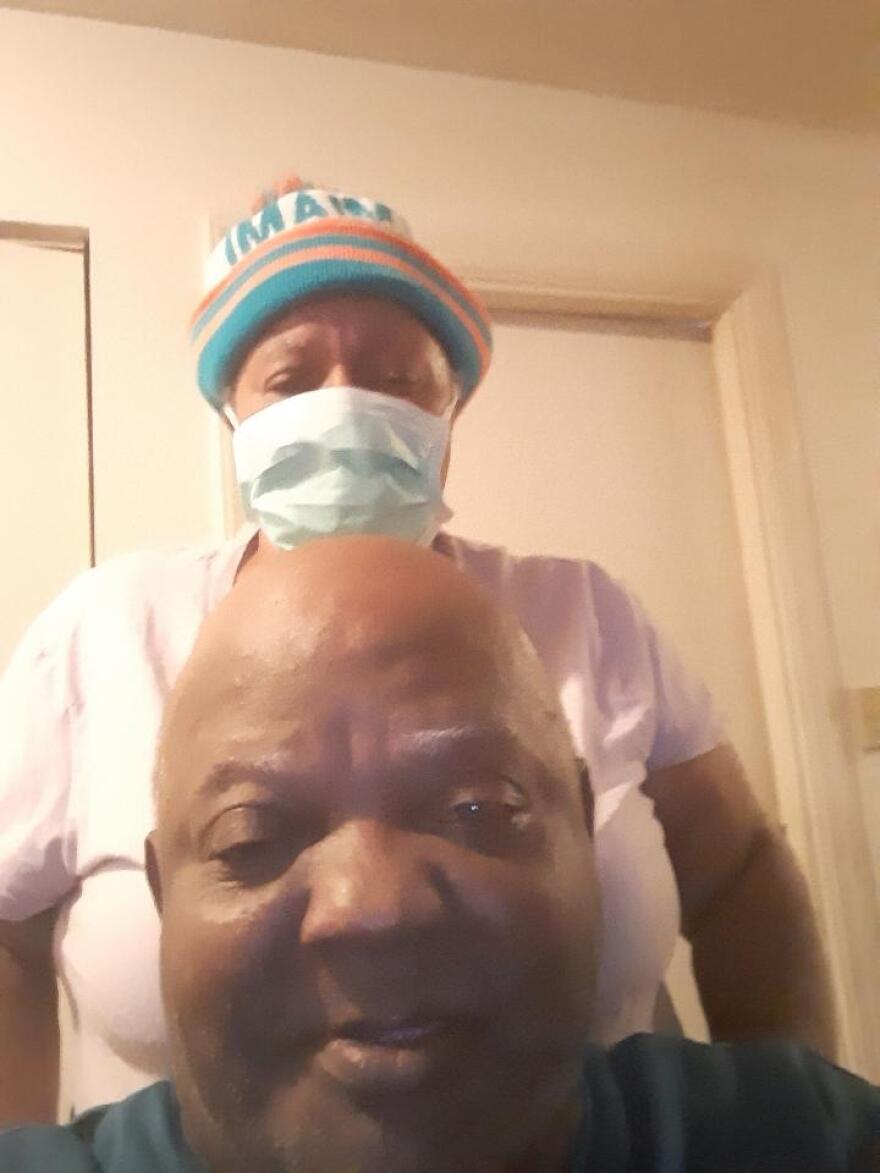
She is taking extra precautions, like always wearing gloves. But when we spoke earlier this week she was down to just ten face masks.
“Sometimes I take the disinfectant Lysol then I’ll just spray it,” Acree said. “I haven’t been throwing them away. After I wear them I go and put them in another ziplock bag… I don’t know how sanitary that is.”
Now advocates for home health workers are concerned they’re not getting the guidance or equipment they need to keep themselves, and their patients, safe.
“There is no social distancing for homecare workers, they are hands-on workers. And they are heroes,” said David Broder, president of Virginia’s chapter of SEIU, a union that helps represent home health workers.
Broder is concerned that if home health workers start getting sick then the spread of the virus could get exponentially worse.
“And yet...they’re lacking personal protective equipment like masks and goggles and face shields, they’re not getting training, and they lack the paid leave that they and their families need to take care of themselves as they’re taking care of others,” said Broder.
What State Officials Can Do
Angelina Drake, with the nonprofit group Paraprofessional Healthcare Institute, says there are steps state leaders can take now to help support home health workers.
One is making it explicit in official documents that home health aides and personal care aides are a part of the essential healthcare workforce. That way they aren’t left out of policy initiatives meant to support those workers.
She also suggests state officials remember home health care agencies when distributing personal protective equipment.
“We understand there’s going to be a level of triage that happens that puts this equipment in the hands of front line hospital and emergency room providers, but the homecare workforce is right behind them,” Drake said. “They’re helping stop the spread and flatten the curve. So if there are resources available these agencies are absolutely in need.”
Short of that, Drake asks for clear guidance from health departments to homecare workers and agencies on things like infection control, and what kind of alternative protective steps they can take if they don’t have gloves or masks.
While the Virginia Department of Health lists COVID-19 resources online for everyone from dentists to emergency responders, there’s currently no information specifically targeted to home health workers.
In the absence, caregivers are figuring things out for themselves. Azza Van De Castle lives in Ashburn and takes care of her 84-year-old mother. She has to go grocery shopping often to meet her mother’s dietary needs, but every trip outside feels dangerous.
“If she died because of me, I will not forgive myself,” Van De Castle said. “(But) who’s going to bring medicine or food?”
So Van De Castle has been covering her face with a scarf and keeping her distance from others when she leaves the house. When she gets home she washes her clothes and immediately showers.
** Updated April 1st, 2020 -- The day after this story initially aired the Department of Health updated resources to include guidance from the CDC specifically for home health workers. On April 1, a spokesperson for the agency also says they'll be distributing masks, gloves and gowns "to home care agencies through the local health districts, based on need and availability." **
This report, provided by Virginia Public Radio, was made possible with support from the Virginia Education Association.